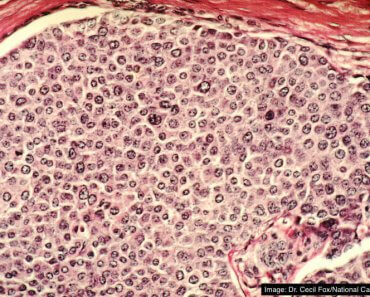
Researchers at Johns Hopkins University have recently discovered that the cell layer surrounding breast milk ducts, called the myoepithelium, works as an active defense against breast cancer metastasis.
Scientists previously believed this cell layer only acted as a stationary barrier to prevent cancer invasion, but in a demonstration with mice, the Johns Hopkins team discovered that it actually reaches out and grabs stray cancer cells to prevent them from spreading throughout the body.
“Understanding how cancer cells are contained could eventually help us develop ways to predict a person’s individualized risk of metastasis,” Andrew Ewald, a professor of cell biology at the university’s School of Medicine and a member of the Johns Hopkins Sidney Kimmel Comprehensive Cancer Center, said in a statement.
The team includes Orit Katarina Sirka, a doctoral student student in Ewald’s laboratory, and Eliah Shamir, who is now a surgical pathology fellow at the University of California, San Francisco.
The research is published in the Journal of Cell Biology.
Myoepithelial layer
Most breast tumors begin in the cells that line the interior of breast milk ducts, Ewald explained.
These cells are surrounded by myoepithelial cells that work to contract and move milk through the ducts when a baby is breastfeeding. This layer is also used to clinically distinguish between contained breast cancers and invasive cancers.
When cancer cells breach the myoepithelium, the result is called invasive carcinoma, which is associated with more aggressive treatment and higher rates of recurrence.
“We knew that the presence and integrity of the myoepithelial layer was key to the clinical management of breast cancer,” said Ewald.
Pathologists like Shamir “diagnose invasive breast cancer based on the presence of cancer cells past the myoepithelium,” he explained.
“Despite this clinical reality, it wasn’t clear whether myoepithelial cells were markers of risk or whether they regulated invasive behavior. Very few experimental systems have modeled the myoepithelium in a realistic fashion,” he continued.
Prior to this study, the understanding of myoepithelium was reminiscent of a castle wall, used as a barrier to block invasive cancer cells, Ewald said.
The study
To determine the functions of myoepithelium, Ewald and his team engineered cells from the lining of mouse breast ducts to produce the protein Twist1, which has been linked to cancer metastasis in multiple tumor types.
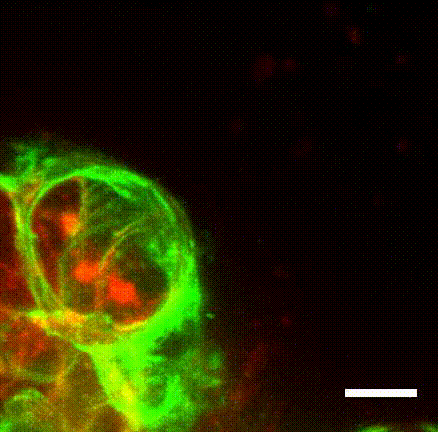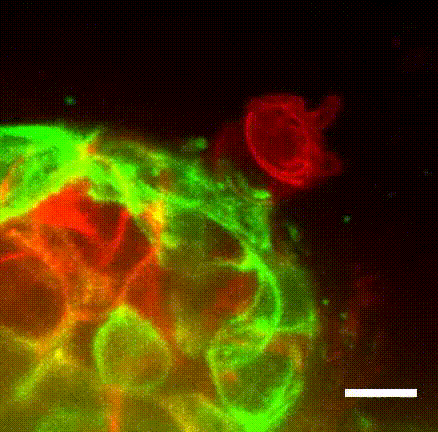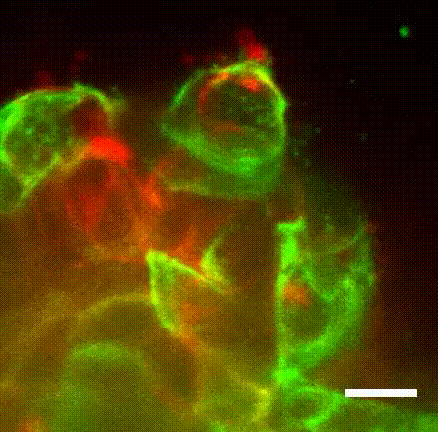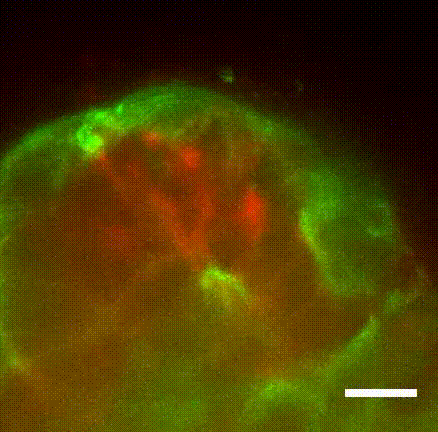
Surprisingly, they found that when the invasive Twist1 cells broke through the myoepithelial layer, the myoepithelial cells grabbed the escaping cells and pulled them back within the breast duct lining.
“These findings establish the novel concept of the myoepithelium as a dynamic barrier to cell escape, rather than acting as a stone wall as it was speculated before,” Sirka said in a statement.
Through 114 observations, the researchers found that this happened 92 percent of the time.
“We were seeing in real-time that the myoepithelium was a dynamic barrier to epithelial invasion,” Ewald said.
“We could literally see myoepithelial cells reach out and grab escaping cancer cells and pull them back into the tumor, thereby preventing their spread.”
Continuing the test
To further confirm this layer was active, the researchers altered two important characteristics of the myoepithelial cells: their ability to contract and their numerical ratio to invasive cells.
They genetically engineered the mice cells to deplete their smooth muscle actin, a protein that enables cells to contract, making it more difficult for them to contract.
Under that condition, the number of escaped invasive cells that broke through the myoepithelial layer increased three times compared to cells with a normal myoepithelium.
The researchers also found that decreasing the proportion of myoepithelial cells to invasive cells increased the number of escaped cancer cells. Specifically, they found that adding two myoepithelial cells for one invasive cell decreases the escape rate four times more than it would with no defending barrier.
“This is important to know because it suggests that both the physical completeness of the myoepithelium and the gene expression within the myoepithelial cells are important in predicting the behavior of human breast tumors. Anywhere this layer thins or buckles is an opportunity for cancer cells to escape,” Shamir said in a statement.
What’s next?
Moving forward, the team plans to study the cellular mechanisms and molecular requirements that prompt the myoepithelial layer to react so dynamically.
“We are working with pathologists to test whether either detection of small breaks in the myoepithelium or molecular analysis of the differentiation state of myoepithelial cells correlate with increased risk of metastatic recurrence,” said Ewald.
“We have also developed genetic approaches to kill myoepithelial cells in an inducible fashion; this will enable us to remove them at different stages of cancer progression and check whether metastasis is accelerated. We are also studying multiple breast cancer models to determine how they subvert this barrier, whether by killing, differentiating, or inducing the escape of myoepithelial cells.”